Education
Learn about our educational philosophy, our curriculum, and what our residents do after residency.
Philosophy
Our primary focus is growth. It does not matter if you are just starting out or if you are a master clinician, our goal is singular — we want you to improve.
Practically speaking, this means that we expect our residents to take on challenges, show us their weaknesses, ask questions, engage in discussion, seek feedback and push themselves to grow.

We approach teaching and learning with a mastery orientation, employing both strategy and effort. We approach all activities, including giving and receiving feedback, with a goal of improving one’s performance. We use experimentally demonstrated strategies to improve teaching and learning. All cases provide opportunities for learning and improving. Failure is another opportunity to learn and improve.”
Keith Baker, MD, PhD
Vice Chair for Education
Integrated intern year
Our new, integrated clinical base year (CBY) will prepare you to succeed. It is a transitional year that pairs traditional rotations such as internal medicine, surgery, and emergency medicine, with integrated rotations where you work with advanced-year anesthesia residents, including acute pain and surgical intensive care. Throughout the year interns will work side by side with their future medical and surgical colleagues while building connections with each other and the anesthesia department. This clinical experience is enriched by a longitudinal, year-long curriculum (one full day every other week on most rotations) that brings the interns together with anesthesia faculty for lectures, skills workshops, and simulation focused on learning relevant to your intern responsibilities and foundational to the practice of anesthesia.
Typical Rotation Schedule
The CBY is divided into 2-week blocks (26 in total). Twenty blocks are spent at the Massachusetts General Hospital, and six at the Newton-Wellesley Hospital to round out your clinical experience.
- 6 blocks of Medicine (including 2 blocks of Bigelow)
- 3-4 blocks of Surgery (including time on the Baker services)
- 3 blocks* of “selectives”, including critical care, consult services, and medical or surgical subspecialties
- 2-3 blocks of Surgical Critical Care (in the Ellison 4 ICU)
- 2 blocks of Emergency Medicine
- 1 block of Perioperative Pain (on the Acute Pain Service)
- 2 blocks* of Anesthesiology (rolling start to “tutorial” at the end of the intern year)
- 4 blocks* of electives, including options like medical education, research through ARC, transfusion medicine, and more
- 2 blocks* vacation – vacation is given in two 2-week blocks
*No weekend or call responsibility
Tutorial
– your “on ramp” to starting residency
At Mass General, you’ll begin with a unique month of tutorial, designed to make the introduction to the field of anesthesia smooth and successful.
During the tutorial month, two staff members are assigned to you. Each staff member will work one-on-one with you for two weeks at a time. This format provides a continuity of learning that allows the you to grow quickly and without having to repeat steps. During tutorial, you are given first choice of cases from the entire operating room schedule, to ensure that you work on cases that match your present level and specific management needs.
Residents start in small groups at staggered times during the summer months, usually 5-6 at a time. This format, along with giving you first choice of cases, allows the tutor/tutee pairs to take part in operating room cases that are appropriate to teach the elementary skills of anesthesia.
During the tutorial month, you’ll also have lectures and an advanced simulation day at the Harvard Center for Medical Simulation. Tutorial will provide you a gentle introduction to the field of anesthesia and prepare you to provide a simple anesthetic to a healthy patient safely.

Rotations
– growth during residency
We take a very deliberate approach to rotation scheduling for our residents. Subspecialties are introduced when you are ready, typically 3-6 months in. By the end of your CA1 year, you’ll have had at least a handful of subspecialties (which we target to your fellowship interests) in addition to at least one of our more complex case rotations, like thoracic or cardiac.
Additionally, each time you revisit a rotation, the cases you are scheduled for should on average increase in complexity. As an example, during the first couple months on General Surgery, our schedulers will aim to get you exposure the full breadth of more common cases, deliberately scheduling you for cases you have not yet been exposed to (e.g., a mix of thyroid cases, breast cases, abdominal cases, etc). When you come back to General Surgery in your CA2 and CA3 years as a senior, you pick whichever cases you want. Or, if you prefer not to pick, the schedulers target more complex cases (e.g., complex liver resections, HIPECs, or patients with more complex comorbidities like LVADs).
First call experience
– your “on ramp” to becoming an attending
The first-call experience is designed to prepare you for independent practice. As first-call resident, you will lead the call team (which includes faculty, residents and CRNAs), allocate resources, communicate with nursing and surgical teams, and manage the ORs overnight. Your first-call attending, who is there with you all night, is your backup and coach for everything you need.
The three main learning goals for the first-call experience are: 1) Administrative: You will learn how to lead and coordinate the OR flow within a large hospital system. 2) Supervision: You’ll get invaluable experience developing plans with residents and CRNAs and then supervising them in the OR. 3) Teaching: You’ll learn what to teach, when to teach, and how to teach.
An attending anesthesiologist is always on call with you and is present for all cases. The role of the attending is to support and teach, allowing you to take the lead and make the transition from resident to independent anesthesiologist. Our alumni tell us that this experience is invaluable after graduation.
Didactics

CBY Series
The Longitudinal Education in Anesthesia Principles (LEAP) series for the clinical base year residents is a full day every other week for our clinical base year residents. It brings the interns together with anesthesia faculty for discussions, skills workshops, and simulation focused on learning relevant to your intern responsibilities and foundational to the practice of anesthesia. The specific curricula within each day include: Lethal Events, Foundations, Non-Clinical Development, Wellness, Evidence, Simulation, Developing Schema, and Skills.
CA1 Series
CA1s have a full day of didactics every four weeks. The integrated lecture series covers basic topics of anesthetic management in flipped-classroom format, including airway anatomy, pharmacology, physiology and physiologic derangements, as well as an introduction to subspecialty anesthesia. These topics are presented in sequence with the goal of building upon a gradually deepening understanding of fundamental concepts. The series also features workshops on airway management, regional anesthesia, and advanced devices.
CA2 Series
CA2s have a full day of didactics every four weeks. The series includes advanced discussions of cardiovascular physiology, lectures on specific cases/events/comorbidities, and small group discussions focused on developing an approach to investigating clinical questions. The didactic days end with advanced workshops, including POCUS, mechanical circulatory support, regional anesthesia, electrophysiology, interventional pain, and more.
CA3 Series
CA3s have a full day of didactics every four weeks. The series includes CA3-led anesthesia presentations, mock orals, mock OSCEs, and a professional development series aimed at important non-clinical knowledge and skills (e.g., personal finance, medicolegal topics, supervising CRNAs, and more). During the last two hours of the day residents who are interested in developing as educators have the opportunity to lead sessions for the clinical base year residents, including simulation, skills workshops, and case-based discussions.
Rotation-Specific Didactics
The Intensive Care Unit (ICU), pediatric, obstetric, neuro, acute pain, chronic pain, preoperative clinic, orthopedic, thoracic and cardiac anesthesia clinical subspecialty rotations conduct weekly didactics, which are in addition to the departmental lectures. This “micro” level of didactic training facilitates case-related teaching. Teams can follow specific cases from the outset, and team members benefit and learn from discussing clinical care decisions with colleagues.
Department sessions
Grand Rounds are an integral component of resident education in the Department of Anesthesia, Critical Care and Pain Medicine (DACCPM). Grand Rounds feature faculty from Mass General, other Harvard-affiliated hospitals, the Massachusetts Institute of Technology, as well as national and international guest lecturers who are leading scientists and experts in their field.
Case Conference is designed for residents to explore actual or theoretical cases based on information taken from a number of medical disciplines. The hour is typically led by a resident with a staff mentor. The goal is to engage in an interactive discussion with the audience regarding preoperative, intraoperative, and postoperative anesthesia care. It provides an opportunity for residents to make key decisions based on the cases that are presented, and to defend their medical reasoning with evidence.
The Morbidity and Mortality Conference is held every two months in place of a Case Conference. This conference provides residents with the opportunity to take part in the department’s continuous efforts to improve quality and safety. Theoretical and actual cases are discussed where near-misses could have resulted in less than optimal clinical outcomes. The discussions are bolstered by literature-based evidence and are aimed at reinforcing the department’s adherence and commitment to safety and safe medical procedures.
Journal Club occurs bi-monthly, providing a format for the residents and faculty to review current literature pertaining to anesthesia practice. The sessions are led by residents and involve an extensive review of the evidence prior to discussing the designated article. The goal of the club is to foster evidence-based practice with critical appraisal of the literature.
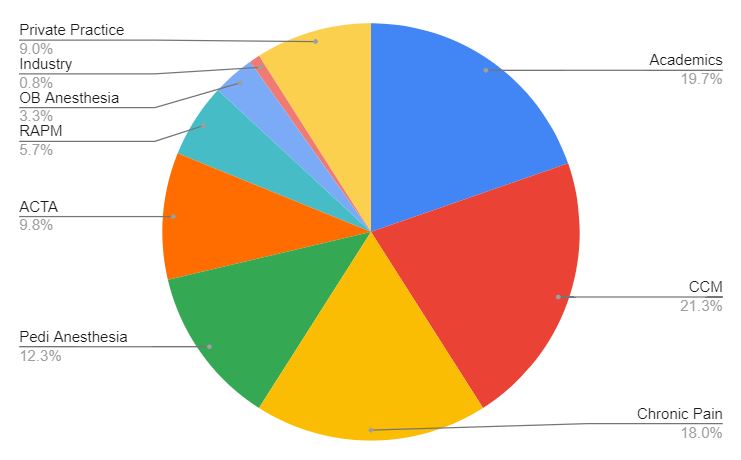
What do our residents do after residency?
All sort of things…