Why MGH?
Educational Culture
Our primary focus is growth. It does not matter if you are just starting out or if you are a master clinician, our goal is singular — we want you to improve.
Practically speaking, this means that we expect our residents to take on challenges, show us their weaknesses, ask questions, engage in discussion, seek feedback and push themselves to grow.
Application of evidence-based approaches to learning is one way that we promote more effective growth for our residents. Retreats and lectures focus on concepts such as deliberate practice, growth mindset, spaced retrieval, and self-regulation.
In emphasizing the development of high-yield learning, our goal is developing master clinicians who continue to grow and pursue expertise long after they complete our Program.
"Deliberate Practice"
Deliberate practice is an effective learning approach that involves systematic, purposeful practice with coaching to improve. It is one of the many strategies we promote to encourage efficient learning for our residents.
“Goldilocks” Learning
The best learning occurs right at the edge of comfort – not too hot, not too cold. This is important in onboarding our residents, giving them progressive challenges during residency, and preparing them for the transition to becoming attendings. To improve learning and smooth out these transitions, MGH offers a unique tutorial and first call experience.
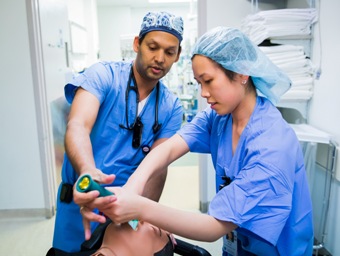
Tutorial
At Mass General, you’ll begin with a unique month of tutorial, designed to make the introduction to the field of anesthesia smooth and successful.
During the tutorial month, two staff members are assigned to you. Each staff member will work one-on-one with you for two weeks at a time. This format provides a continuity of learning that allows the you to grow quickly and without having to repeat steps. During tutorial, you are given first choice of cases from the entire operating room schedule, to ensure that you work on cases that match your present level and specific management needs.
Residents start in small groups at staggered times during the summer months, usually 5-6 at a time. This format, along with giving you first choice of cases, allows the tutor/tutee pairs to take part in operating room cases that are appropriate to teach the elementary skills of anesthesia.
During the tutorial month, you’ll also have afternoon lectures, a full simulator course and an advanced simulation day at the Harvard Center for Medical Simulation. Tutorial will provide you a gentle introduction to the field of anesthesia and prepare you to provide a simple anesthetic to a healthy patient safely.
Rotations at "Just Right" Levels
When you first learn to drive, you don’t hop in a stick shift and try to drive through a snowstorm, right? Conversely, if you are a master driver, you probably won’t be pushed to grow with a quick circle around the block.
We take a very deliberate approach to rotation scheduling with our residents. Subspecialties are introduced when you are ready, typically 3-6 months in. By the end of your CA1 year, you’ll have had at least a handful of subspecialties (which we target to your fellowship interests) in addition to at least one of our more complex case rotations, like thoracic or cardiac.
Additionally, each time you revisit a rotation, the cases you are scheduled for should on average increase in complexity. As an example, during the first couple months on General Surgery, our schedulers will aim to get you exposure the full breadth of more common cases, deliberately scheduling you for cases you have not yet been exposed to (e.g., thyroids, breast, abdominal, etc). (They refer to this as making sure your passport gets all the stamps.) When you come back to General Surgery in your CA2 and CA3 years as a senior, you get to pick whichever cases you want. Or, if you prefer not to pick, the schedulers target breadth, but this time with more complex cases (e.g., complex liver resections, HIPECs, or patients with more complex comorbidities like LVADs).
First-Call Experience
The first-call experience is designed to prepare you for independent practice. As first-call resident, you will lead the call team (which includes faculty, residents and CRNAs), allocate resources, communicate with nursing and surgical teams, and manage the ORs overnight. Your first-call attending, who is there with you all night, is your backup and coach for everything you need.
The three main learning goals for the first-call experience are: 1) Administrative: You will learn how to lead and coordinate the OR flow within a large hospital system. 2) Supervision: You’ll get invaluable experience developing plans with residents and CRNAs and then supervising them in the OR. 3) Teaching: You’ll learn what to teach, when to teach, and how to teach.
An attending anesthesiologist is always on call with you and is present for all cases. The role of the attending is to support and teach, allowing you to take the lead and make the transition from resident to independent anesthesiologist. Our alumni tell us that this experience is invaluable after graduation.
Robust Clinical Experience
Massachusetts General Hospital admits more than 48,000 inpatients annually. Our patients are often complex and acutely ill. Similarly, many of the operative cases are quite involved. Challenging cases include solid organ transplants (e.g., heart, lung and liver), penetrating and blunt trauma (Mass General is a Level I trauma center), open major vascular, complex thoracic, and more.
Residents are given a level of supervision appropriate to their level, along with a caseload that provides a broad clinical experience. Our goal is to always have the resident in the “driver seat” but with ample support. These cases are challenging but we provide you the support you need to achieve — another example of “Goldilock” learning. This quickly builds technical expertise, good judgment, leadership and decision-making skills, allowing residents to become confident in dealing with the most challenging perioperative issues.
In addition to caring for patients in the operating room, residents learn to manage perioperative cases in the intensive care unit (ICU), recovery room, neuroradiology suite, proton therapy center, MRI suite, endoscopy suite, and electrophysiology and cardiac catherization labs.

Extracurricular Opportunities and Support
The Program offers robust support to help our residents develop complementary professional skills.
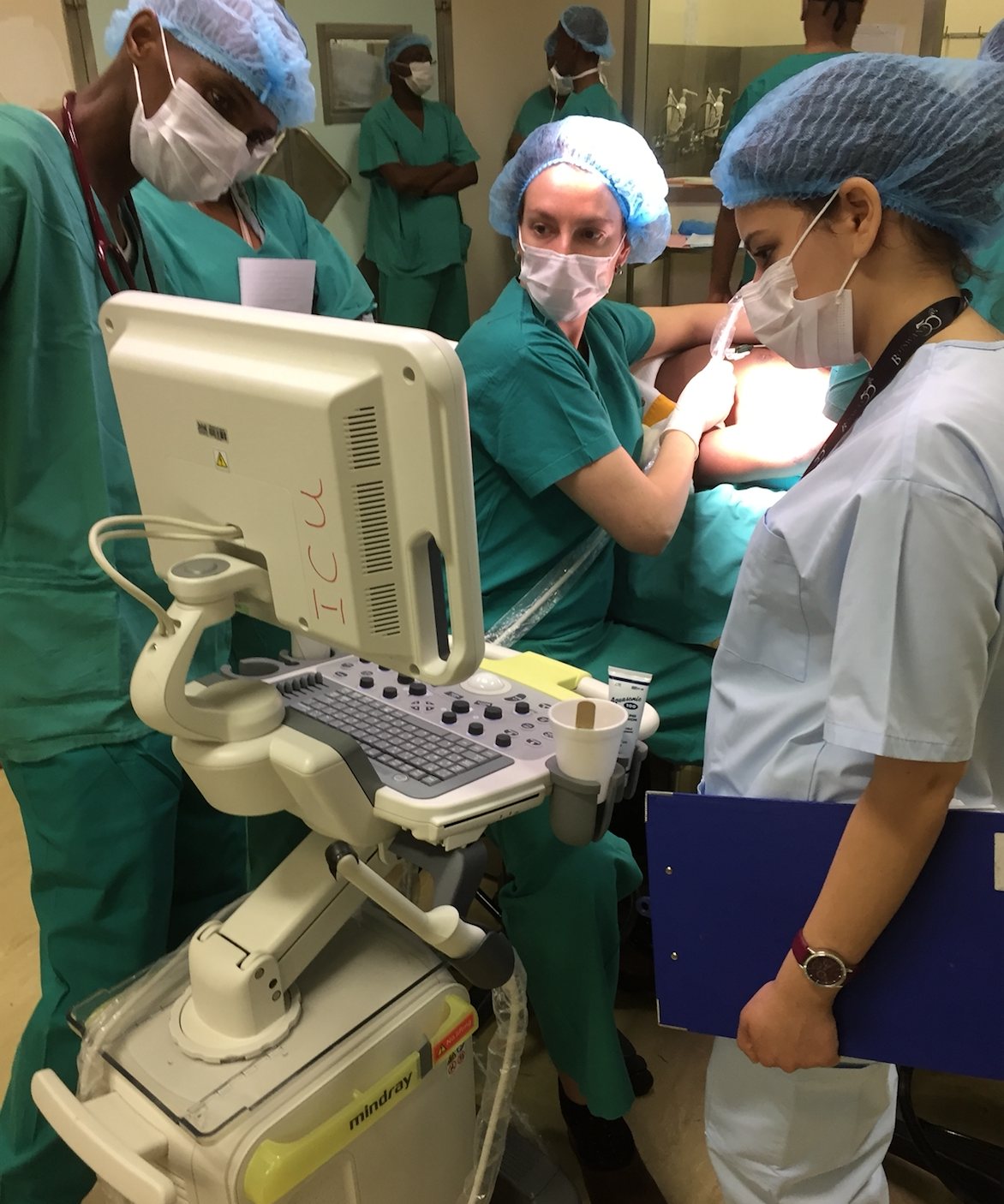
Dr. Devan Bartels, teaching ultrasound in Botswana
Research
The DACCPM has an exceptional record of developing young physician-scientists to become innovators and research leaders. The meshing of patient care and medical science at MGH results in the rapid translation of new scientific ideas and developments (such as inhaled nitric oxide, short acting nondepolarizing muscle relaxants and new medical devices) into practical applications that help patients worldwide. The MGH receives more NIH research funds than any other independent teaching hospital. Read more about our department’s research effort here.
During residency, we provide support in a variety of structured and unstructured ways to help develop our residents as investigators and scholars.
- Our Travel Support Program provides financial assistance to cover costs of meeting travel, lodging and registration for participating residents. Residents participating in any capacity can take advantage of this during residency. Residents who are presenting original research can take advantage of this yearly.
- Established by a generous alumnus donation, the Levy Resident Research Grants aim to support the career development of outstanding DACCPM Residents who wish to improve patient care through research. Designed to emphasize the importance of a mentored research project, recipients receive guidance and up to $3,000 to support each research effort. In order to provide residents experience applying for funding, the process is intended to model that of a typical grant application.
- Our CA3 Research Track comes with six months dedicated to research during the final year of residency. These robust offerings are complimented by our top-notch statisticians, an innovations lab and engineering group, and plenty of opportunities for presenting your work. This program is designed to function as an on-ramp to a career as a clinician-scientist. Those interested in starting as faculty on a T32 should have little difficulty making the transition with this offering.
- Should you choose to stay at MGH as new faculty, one of our mechanisms for fully developing your research potential is our Mentored Scientist Research Track – an NIH funded Training Grant (5T32-GM007592), which currently supports seven trainees in Harvard anesthesia departments. Trainees spend 75–80% of their effort on research (required by NIH). Though most trainees choose mentors at Harvard Medical School, one of its affiliated hospitals, or at Massachusetts Institute of Technology, we are extremely supported of investigation and encourage individuals to select any mentor in the Boston. Most of our Training Grant alumni continue on in research with additional mentoring during early-stage research career development. Over 85% of T32 program alumni over the last 15 years have obtained independent external funding for their research.
Patient Safety & Quality Improvement
We have many offerings for those interested in QI and patient safety.
- Our residents have access longitudinal online spaced education course in patient safety and quality improvement. This weekly online course takes our PGY-1s and CA-1s through 8 vignettes to teach them about the important aspects of the field.
- Our CA1s each participate in a QA Committee meeting to better understand this process, DPH reportability and root-cause analysis.
- Our curriculum includes an experiential QI group project that residents will participate in during their CA2 and CA3 years.
- To complement our departmental M&M format, our residents created “Resident M&M,” a novel resident-centered, resident-organized monthly M&M conference that provides an alternative forum for residents to present their own cases to their peers. Residents report high satisfaction with these sessions, and have identified multiple systems issues that have spawned numerous resident-led quality improvement and curriculum development projects.
For residents who want to take it to the next level:
- We have paid for free access to all Institute for Healthcare Improvement courses.
- Residents can join our highly networked Center of Expertise in Healthcare Quality and Patient Safety, a center that is designed specifically to develop trainees across our institution with the tools and connections to be successful in QI and patient safety.
- You can apply to join the Department’s Quality and Safety Improvement Committee (QSIC), a process improvement group comprised of faculty, fellows, residents, CRNAs, nurses and administrative staff. It is very common to have device inventors, pharmacists and health information technology experts participate for input and collaboration. Learn more about this group in the article linked here (PubMed login required).
- You can participate in a QI Elective month. Residents who participate are mentored by the heads of the QA and QSIC Committees. The month is comprised of a set of specified readings and a resident-led project.
Check out this video, highlighting one of our recent resident-led QI initiatives, which won the national Anesthesia Patient Safety Foundation Resident Quality Improvement Award.
Global Health
We have a number of incredibly invested faculty who have built their careers around Global Health, including joining to our highly networked Center of Expertise in Global and Community Health, a center that is designed specifically to develop trainees across our institution. Interested residents can participate in one of two different types of Global Health experiences.
- Shorter trips: The focus of these 1-2 week trips is the provision of anesthesia care to overseas patients in need.
- Longer trips: These one-month trips focus on educating local caregivers to improve the quality of care for patients in the area long-term. These trips are co-sponsored by the SEA-HVO.
Recent international rotations have taken residents to countries including Botswana, Uganda, Rwanda, Ethiopia, the Philippines, China, Vietnam, Columbia and Peru.
There are two main scholarships offered nationally for anesthesiologists interested in Global Health, the SEA-HVO award and the ASA-GHO award. This past year, both were awarded to residents at MGH!
Medical Education
The Program offers several mechanisms for developing skills in medical education.
Informal opportunities include intra-operative teaching of our medical students during their anesthesia rotation, onboarding of our new residents prior to their one-on-one Tutorial, teaching and supervision of junior residents when taking on the First Call role, and plenty of didactic presentation opportunities.
Residents with deeper interest have a few more options:
- Harvard Macy Course for future academic clinician-educators: A three-day intensive course on skills in teaching and learning AND developing scholarship in medical education. Residents can apply Travel Support funding to cover the cost of participation in this program.
- Simulation Elective at the Center for Medical Simulation: This one-month senior elective allows interested residents immersive training in simulation and debriefing at this world-renowned facility.
- The Center of Expertise in Medical Education offers a number of resources to help promote education, education scholarship and education administration, designed specifically for trainees at our institution.
- Additionally, residents interested in Medical Education Scholarship can collaborate with one of several medical education researchers in the department.
Perioperative Administration
In addition to the first call role, senior residents who wish to take this to the next level can participate in a focused one-month long Perioperative Administration Elective, which allows residents a much deeper experience with many facets of administration. These include areas such as strategic planning, budget planning, and hospital resource triage.
Residents can also join the Center of Expertise in Health Policy & Management which is designed specifically for trainees to gain management in administrative and policy leadership in healthcare.
Elective NOS – an active role in customizing your educational experience
In addition to elective months, residents get a number of days throughout residency (called “Elective NOS” days) where they can select the learning experiences that best fit their needs.
CA1s can pick any OR or non-MOR anesthetizing site where an attending is scheduled to work alone. They then get dedicated one-on-one teaching with that attending with the location and cases they picked!
CA2s and CA3s can pick from a number of other options including a day doing awake bronchoscopy in the internventional pulmonology clinic, a day performing root-cause analysis on an actual OR case, an administrations/operations day with our Associate Director of Perioperative Services, a day with the cardiopulmonary perfusionists, and more.
“Elective NOS gives dedicated and extensive attending teaching time, direct observation of my technical skills and decision-making with immediate feedback.”
“I made the best of a day without many awake bronchs — [attending] gave me a talk on trachs and we spent time with the simulator. Very useful overlap with anesthesia and a valuable day for residents.“
“I learned about QA processes and how to perform RCA. Helpful to discuss steps of completing RCA and creation of fishbone diagrams. Also just helpful to be able to discuss RCA, just culture, peer support.”